Has it really been over a month since I last blogged about Ellie's sleep issues??? Apparently, it has. This is where we left off: Treatment plan and health risks associated with obstructive sleep apnea [OSA]. To learn more about Ellie's sleep issues, read here. But first, a few little photos from Easter:
We finally got in to see Ellie's ENT doc at the beginning of March. Her sleep specialist fought to get her an appointment back in mid-February, but the ENT was out of town. Anyway, the purpose of the ENT appointment was to evaluate whether or not Ellie's adenoid had grown back. If so, we would then proceed with a repeat adenoidectomy (because surgery is so much fun!) in hopes that would "cure" her OSA and "oxygenation instability". I had 2 choices: lateral neck x-ray or a flexible nasal laryngoscopy. I went with the laryngoscopy. Yes, it sounds mean, but it is quick. It provides more detail information. Plus no radiation is involved. Plus, I have this perverse obsession with seeing people's insides (it is the nurse practitioner in me - especially being a former ENT NP).
 |
| Ellie's procedure was the pic on the right. |
This is how it went: the nurse kindly sat with Ellie. Her legs over Ellie's and her arms around Ellie's. I then stood behind the nurse with my hands holding Ellie's head straight. Now, a laryngoscope is essentially a spaghetti-like noodle with a camera on the end. It passes through the nose and looks at the structures of the upper airway. It can be used to diagnosis enlarged adenoid and tonsils, enlarged base of tongue, laryngomalcia (floppy airway), abnormalities of the vocal cords, and even reflux. How did Ellie Bear do, you ask? Well, she fought it all while screaming "NO THANK YOU! NO THANK YOU! NO THANK YOU!" Girlfriend is nothing, but polite.
The findings were not what I was hoping for. It may sound strange, but I wanted that adenoid to be there. She is obstructing. She has had nearly nonstop sinus infections again since August. If it had regrown, we could have "easily fixed" it. Nope. The adenoid did not grow back. While she does not have an abnormally large tongue, she does have a large tongue base. She also has not only a high arched palate, but a long palate that dips into the upper airway. At rest, between the tongue base and the palate, she is already in a partial obstruction - this is while awake and upright. With sleep, the muscles relax and while laying down, it allows everything to collapse back into her airway. We also learned that she had reddening of the epiglottis suggesting reflux. Goody.
 |
| Depicts large tongue base causing obstruction of air flow Photo courtesy: Dental Magazine - unable to find vol # |
Take the above pictures and add it to the pic below and that is Ellie's anatomy
 |
| Depicts soft palate obstructing air flow |
So guess what we have been doing these past few weeks? CPAP mask desensitization! The fun never stops. By the time all was said and done - the doc writing the script, insurance approval, equipment ordered, and equipment training, we finally started on March 26th to desensitize Ellie towards wearing her CPAP mask. Let us pause for a moment to think about how that. Desensitize. Ellie. Is it going to take years like bath desensitizing did? Save me now!
 |
| It's Fighter Pilot Mickey |
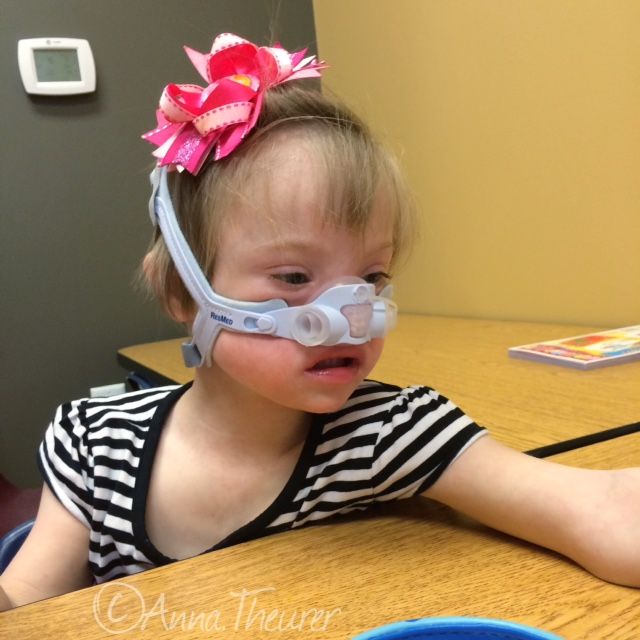
Continuous Positive Airway Pressure [CPAP] is considered to be a type of ventilation therapy in which positive pressure is blown into the airway as a treatment for obstructive sleep apnea. We are trying what is called a "Pixi" mask. This is a mask that fits over her nose only, as opposed to a mask that fits over both the nose and mouth. You need to create a tight seal or otherwise the pressurized air will leak around the mask. If she starts to mouth breath, the air will escape so there is a strong possibility she will need the full face mask.
You can just imagine how this is going. My daughter has some significant sensory avoidance issues when it comes to her face, hair, and head. Tooth brushing requires some interesting gyrations, which involve my legs over hers and my arm holding down her arms. Combing or washing her hair is considered a form of torture. Now she has to wear a mask over her face? One that blows pressurized air into her face? Right. . .
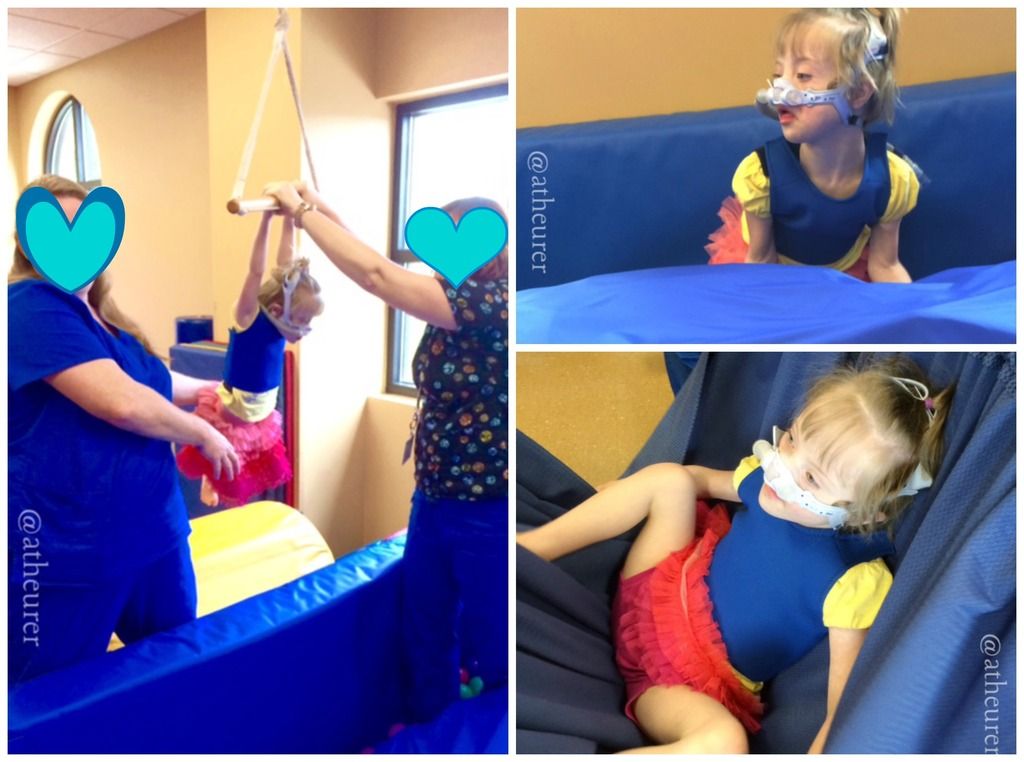 |
| Co-therapy between speech therapist and occupational therapist in the sensory gym. Also trying out a compression vest since Bear has been behaving like the Tasmanian Devil on steroids. |
So desensitizing is a s l o w process. A step by step approach. Ellie is to build up to wearing her mask for 15-20 minutes, 3 x day. Then we add hooking it to the machine and turning it on - again 15-20 minutes, 3 x day. After that, falling asleep with the mask hooked up to the machine and turned on. We are making progresses. . . sort of.
 |
| "yeah, I'll totally wear it if Papa is next to me." |
At therapy (ST/OT), she will wear the mask without too much difficulty. She has worn it for 2 therapy sessions for ~30 minutes! At home, she will touch it, but shout "NOOOOO!" when she sees me hold it. She will allow Mickey Mouse to wear it. She will try to put it on Minnie Mouse. Once, she tried to put it on herself - in the waiting room at therapy. Apparently, she associates therapy with the CPAP mask now. Once, she allowed me to put the mask over her face just before we went for a ride in the car. I am also able to place the mask on her once she is already asleep, but am not able to turn on the actual CPAP. Progress is progress. No matter how slow it is.
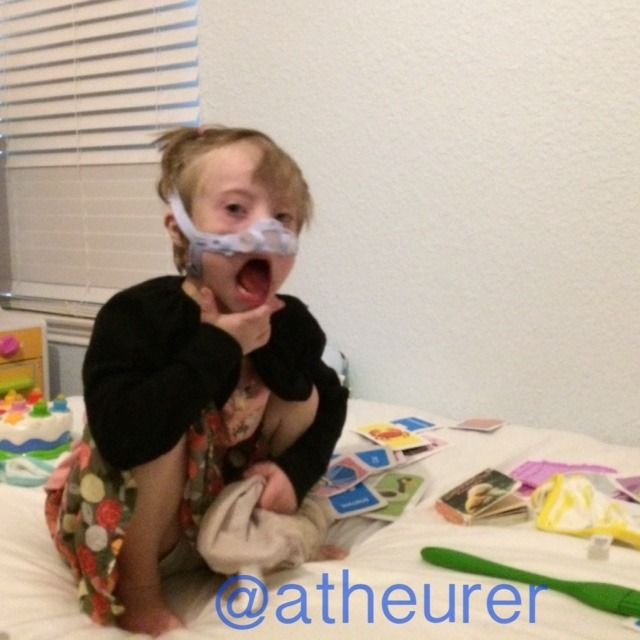 |
| Traitor! You said this would be fun. You said I was going to be a fighter pilot. |
Our sleep doctor told us to follow up in 2 months time. It is said that if she will not wear the mask with CPAP within 2 months, she will most likely never wear the mask (well at least in the near future wear the mask. Maybe in 10 years she'll wear it, but that doesn't really help the now). That means Ellie would have something called a Cine MRI, which is basically an MRI in motion to look at the airway while the patient is under deep sedation. The Cine MRI helps determine if surgery is necessary and if so, what part of the upper airway needs to addressed. So yeah, I want the CPAP to be tolerated and to work.

Follow us on Facebook! http://www.facebook.com/annatheurerfitness http://www.beachbodycoach.com/annatheurer https://www.facebook.com/pages/The-Chronicles-of-Ellie-Bellie-Bear/216738345037166
 |
| My little dancer who recently discovered her shadow. |

Follow us on Facebook! http://www.facebook.com/annatheurerfitness http://www.beachbodycoach.com/annatheurer https://www.facebook.com/pages/The-Chronicles-of-Ellie-Bellie-Bear/216738345037166




Ugh. That sounds….
ReplyDeleteOk, I've got nothing constructive.
Sounds like it sucks. Sending love & hugs & wine!
a condition in which too many growth hormones are released into the bloodstream, Sleep Apnea Blueprint
ReplyDeleteIt really stinks that Ellie has to go through this. However I think it is great that you are taking her to doctors and trying to do anything to help her with it. It is even more amazing that she understands that she has to wear it and that It no longer bothers her much.
ReplyDeleteCynthia Bowers @ Bay Area TMJ & Sleep Center
Thanks for sharing as it is an excellent post would love to read your future post.
ReplyDeleteSS Technomed offer you Double Surface Phototherapy Unit or Bubble Cpap Machine at best price.
I got too much information from this post which I wanted for CPAP masks .
ReplyDeleteThank you for another timely and informative article on CPAP machines. It’s incredibly helpful, and I’ve gained valuable insights from this blog.
ReplyDelete