Sleep Study Results Revealed and Explained
We have known about Ellie’s sleep study results for about a week now. There has been a lot of information to process and of course, a lot of researching on my end. (Hey, I used to order sleep studies, not interpret them!)
Oh where to begin. For a recap of her sleep issues, visit here. For more information about the sleep clinic appointment, visit here.
 |
| My little sleep deprived movie star. |
According to the doctor:
“Ellie is a 5 year-old with trisomy 21. She has evidence of mild pediatric obstructive sleep apnea. However, the patient has evidence of nocturnal hypoventilation and moderate-to-severe oxygenation instability as a result of her sleep disordered breathing. She requires intervention for her OSA.”
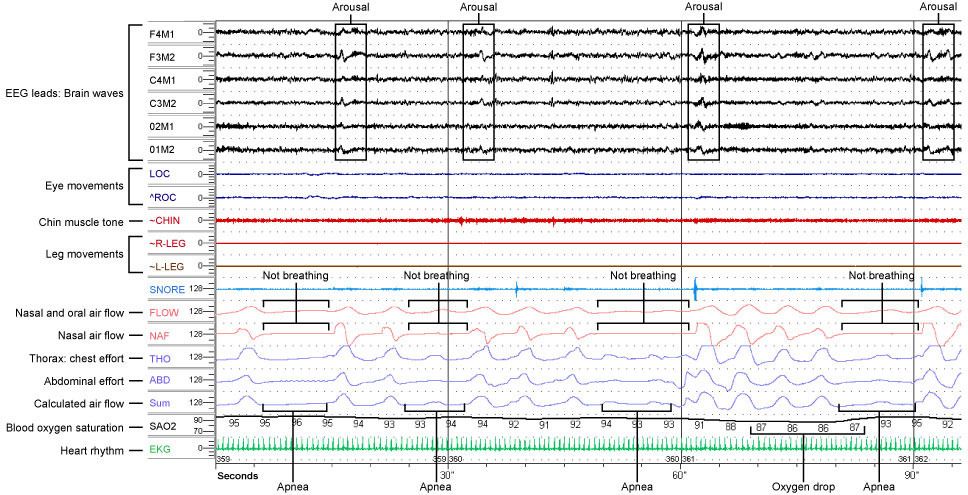 |
| Polysomnography showing apnea with oxygen desaturations and arousals following apnea. Photo: www.northcountryneurology.com |
Translation:
Ellie sometimes stops breathing while she sleeps aka has apnea. According to her sleep study report, she only had 3 apnea episodes, each lasting approximately 10 or more seconds. It is obstructive because her physical anatomy (small mid-face, tongue, palate, etc) affects her ability to breath while laying down. Central apnea would involve a problem with the brain signaling the chest muscles to move and this type of apnea has been ruled out. Pediatric apnea is defined as a pause in breathing. In children, the pause can be any length of time while in adults, apnea is defined as pauses in breathing that lasts ≥ 10 seconds.
Hypoventilation is the reduction of airflow by 50% for two respiratory cycles accompanied by reduction of saturation by 3% or arousal from sleep. Right. So in layman’s terms, the amount of air that flows into the lungs is 1/2 of what it should be and as such, her oxygen saturations [SpO2] go down.
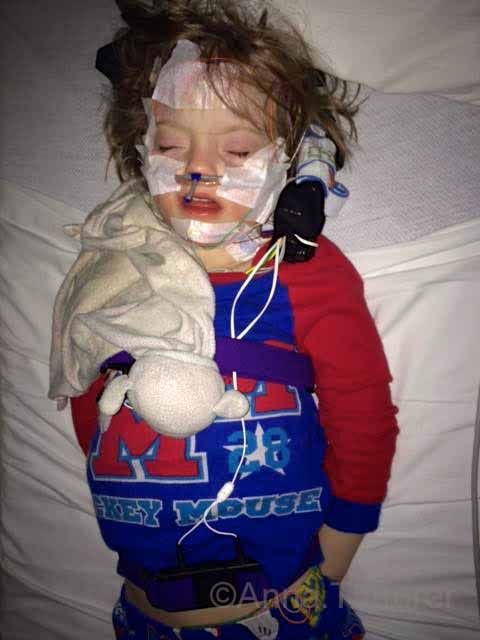 |
| Ellie's overnight sleep study. How can one sleep with all those wires? |
Respirations, Carbon Dioxide, Oxygen Saturations:
Ellie is diagnoses with nocturnal hypoventilation because she takes very few breaths while asleep and those breathes are very shallow aka she has hypopnea. Each hypopneic episode lasted 20 + seconds. This causes poor inhalation and exhalation as well and a decrease in oxygen saturation.
Oxygen Saturations: looking at oxygenation levels during hypoventilation. Say that Ellie’s normal O2 sats are 100% (okay, her sats really do sit at 100%), if she drops to 97%, it is logged as hypoventilation ( or say when she dropped into the 80’s as seen during her sleep study).
Carbon Dioxide Levels: Breathing also involves the exchange of oxygen and carbon dioxide [CO2]. As you breath O2 into the lungs, you expel carbon dioxide out through your nose and mouth, My daughter’s inhaled CO2 levels are very high. For 81% of the time she is asleep, her CO2 levels are 50-62mmHG. Normal CO2 is 35-45 mmHg. Think of it as breathing face down into a pillow . . . for a huge chunk of the night.
Respirations: A normal respiratory rate for a 5 year-old is ~ 20 breaths per minute. While asleep, Ellie’s was at 9-12 breaths per minute. Too few breathes = hypoventilation = increase CO2 + decreased O2
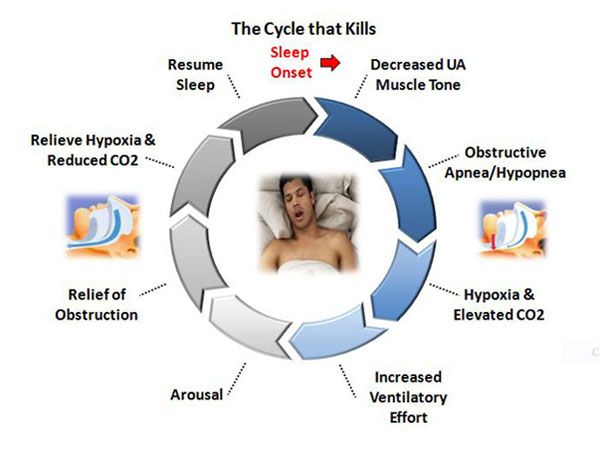 |
| Photo: www.proacthealthsolutions.com |
Quantity vs. Quality and Arousal.
It should be noted that Ellie managed to sleep 7 hours and 48 minutes during her sleep study. She fell asleep quickly and her arousal index was 15.1 (normal 9-16). She spent 33.3% in REM sleep which is age-appropriate. All of this is good, except REM sleep is where everything goes down hill. Here is how it goes, your brain recognizes that your CO2 levels are rising, this causes an arousal. With that arousal, you wake up a bit and trigger a bigger inhalation of air and thus increase your oxygenation and bring down the CO2 from the danger zone. This is why people who have apnea tend to wake up alot through the night or never feel rested during the day. Even if the quantity of sleep is there, the quality is not.
Indexes Defined:
Apnea Hypopnea Index [AHI] looks at the number of apneas and hypopneas per hour of sleep. For Ellie, her AHI was 4/Hr which placed her at mild OSA. However, during REM, her AHI was >12/Hr which is severe.
SpO2 nadir is a fancy way of saying “the lowest SPO2 recorded”. Ellie’s lowest sat was at 81%. This is not good, but it didn’t require intervention with supplemental oxygen during the sleep study.
Oxygen Desaturation Index [ODI] looks at the number of times per hour, a person’s oxygen saturations drop by 3% or more. For Ellie, her ODI was 6.8 during stage 1&2, but then jumps to 9.5 ODI during REM sleep. This is another reason why she has “oxygenation instability”.
 |
| Someone thought that should would take a little rest during dance class. |
This blog post is turning into a term paper here so I will sign off now and write another post later on what the plan is for Ellie.

Follow us on Facebook!
http://www.facebook.com/annatheurerfitness
http://www.beachbodycoach.com/annatheurer
https://www.facebook.com/pages/The-Chronicles-of-Ellie-Bellie-Bear/216738345037166



Very interesting. My daughter had a sleep study a week or two before Ellie, and she has "Mild Sleep Disordered Breathing." They are not recommending intervention, but we are doing palate expansion soon to hopefully open up her airway. She consistently wakes up one to three times per night and is tired during the day.
ReplyDeleteI also have been meaning to get in touch as you inspired me to start PiYo and Shakeology. I tried to choose you as my coach, but it didn't work so I have someone randomly assigned to me. I would love for you to get credit for my monthly purchases... What do I do?
Hi Erin, I apologize it has taken me so long to get back with you. You will have to let me know how the palate expansion goes. Is it a surgery or is it some appliance that you put on the roof of her mouth? I just cannot imagine so much interrupted sleep--for your daughter and for you! Sleep deprivation is miserable for all involved :-( With Ellie, we are checking for adenoid regrowth and if they grew back, our first line of treatment would be to remove the adenoid again. After that CPAP. If CPAP isn't tolerated, then possible palate or tongue advancement surgery. I am not thrilled!
DeleteI am so happy that you are doing PiYo and Shakeology! I love love love PiYo and I kid you not that it has really helped my back. What do you think of it so far? I do love Shakeology and drink it everyday for breakfast. To transfer over to me, you would want to call customer service: 1-800-470-7870. Tell them that you would want to switch to Anna Theurer with Coach ID: 410279 It should only take about 2 minutes. Now, if you'd like friend me on Facebook (Anna Bruns Theurer) in Austin, TX. I offer an accountability and challenge group for people who have me as their coach. It is a lot of fun and is such a great place for support, encouragement, and motivation :-)
The palate expander is an appliance. Carrigain will do rapid expansion for 1 month, and then wear the device for 6 months to maintain the space. We don't have it in yet, but I'll let you know how it goes. Most dentists/orthodontists like to wait for 6 year molars to come in, but there is a way to do it with younger children.
DeleteI just contacted customer service about switching to you. I am loving both the PiYo and the Shakeology. I too have some back pain, and that's one of the reasons I wanted to try PiYo. For the most part it's been fine, but in the past couple of weeks, I've had some increased pain. I think my hamstrings/hips are tightening up after my workout and pulling my back out of alignment. That used to happen after running sometimes too. I obviously need to stretch more! I have one day left on my PiYo 8 week calendar, and I may be in touch about what to do next...
Goodness, I am horrible about replying to comments! I will be interested in seeing how Carrigain handles the appliance. It looks like we are going for CPAP first :-/ Not fun for either one of our girls!
DeleteFor your hips- pigeon pose! It stretches your hip flexors which are key to eliminating tightness and helping pull your spine into proper alignment. Straddle stretch is great for the hamstrings as well. :-)
I definitely enjoying every little bit of it. It is a great website and nice share. I want to thank you. Good job! You guys do a great blog, and have some great contents. Keep up the good work.
ReplyDeletesleep ressearch
wow this good but ,I like your post and good pics may be any peoples not like because defrent mind all poeple ,
ReplyDeletesleep ressearch
Oh I cheated now and then, but I sure tried to be good to no avail. There is good news. sleep apnea blueprint article
ReplyDeleteBecause of this many people are left anxious and clueless about what went wrong, and not just that, it makes them hesitant in hiring an escort again. Austin strippers
ReplyDeleteA good blog always comes-up with new and exciting information and while reading I have feel that this blog is really have all those quality that qualify a blog to be a one Colorado Strippers
ReplyDeleteExcellent article. Everything here is just as I expected it to be. It's even better than that. The information here helped me to complete my paper on this topic. Thanks for that. Continue to write more articles like this Denver Strippers
ReplyDeleteAppreciating the time and effort you put into your site and in depth information you provide. It's great to come across a blog every once in a while that isn't the same old rehashed information. Great read! I've saved your site and I'm adding your RSS feeds to my Google account. polissonografia brasilia
ReplyDeleteI'm very enjoyed because of this blog. Its an educational topic. It help me very much to fix some problems. Its opportunity are so fantastic and working style so speedy.ronco apneia brasilia
ReplyDeleteSinusite tem Cura? Há mais de 10 anos tratando Otorrino em Brasilia. A clínica possui expertise para o tramento da Sinusite em Brasilia. Sinusite brasilia
ReplyDeleteI found your this post while looking for details about blog-related research ... It's a good post .. keep posting and updating information.polissonografia asa sul
ReplyDeleteVery nice blog post, thank you for share your great idea.
ReplyDeleteSleep Apnea Treatment,Sleep Apnea