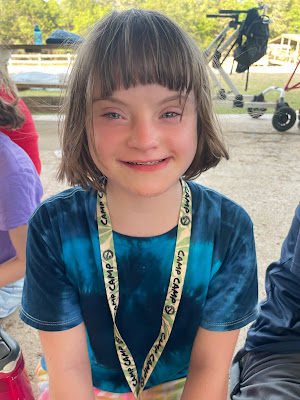
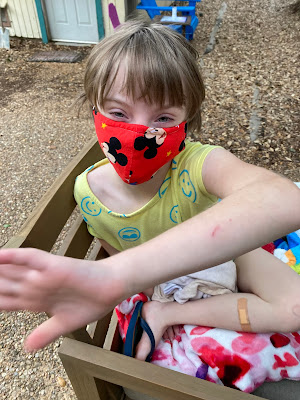
Here we are - two posts in 30 days! It's scandalous, I tell you! Seriously though, I bet you all thought that I abandoned ship and would revert back to neglecting this blog. Well. . . ahem, *whispers* I thought about it, but then I figured I'd present you with more random medical stuff, some pics, and the usual Ellie Bear antics. Yes, antics on steroids because you know, hormones and puberty.
If you've been following The Chronicles of Ellie Bellie Bear for a while, you know that I love to get into all things medical. I am a former pediatric nurse practitioner turned mama bear to a sassy 13 year-old with Down syndrome and other random, semi-complex, but not serious medical issues that pretty much have nothing to do with her having Ds. Please the disclaimers listed on the side of my blog.
Now on to the actual point of this post. There is a point? In case you cannot tell by the title, Twinkletoes still has her cecostomy and for the most part, it has been a Godsend as her constipation is finally well controlled and she is no longer fighting us with the ante-grade enema administration. She seems to be happier now that she doesn't have weeks'-worth of stool packed into her gut and she is eating better and finally no longer failure to thrive. It took us some time to find a good regime and we have to tweak it here and there but she is now getting 175cc of SMOG through her tube 3 x week. SMOG is saline, mineral oil, and glycerin. Sometimes we toss some Milk of Magnesia directly through the tube if she seems to be getting backed up. The type of enema through a cecostomy is different for everyone -some people only need water, others need saline, etc. We were hoping that she would only have it for 2 years to allow her colon to snap back to its original size and elasticity but here we are 6 years later and she just cannot seem to go on her own. The kiddo may be a cecostomy lifer and I am actually okay with that.
That being said as with any ostomy and with any medical device (Chait Trapdoor), there can be things that go wrong. The list includes infection, appliance failure, skin breakdown, infection, parastomal hernia, and tube dislodgment.
**Even with all of the possible complications, I firmly believe that for Ellie, this cecostomy has vastly improved her quality of life and my husband and I do not regret her undergoing this procedure.
Photo Credits:
Left: Cook Medical
Right: Arya, Shruti & Gupta, Nancy & Gupta, Rahul & Aggarwal, Arun. (2016). Constipation and Outcomes of Cecostomy. American Journal of Therapeutics.
Ellie has what is called a Chait Trapdoor. It is a rectangular-shaped button that sits flush with her abdomen. The tube itself has a straight piece turning into a "pig tail" or corkscrew. This tube is typically replaced under fluoroscopy with sedation every 9-12 months. Ellie spends more time in recovery than the length of the actual procedure. The usual risks include bleeding, infection, device failure, and gut perforation. I think she has had it replaced 6 times. One for each year and then a little extra one from way back in the day when the Princess StinkyPants pulled the tube out.
Taken a few years ago, this is how the Chait Trapdoor should look.
Photo Credit: Science Direct
*Some of the images in this post may be considered graphic by some.*
WHEN THE TUBE IS TOO LARGE
For years, the tube was the perfect size sitting flush to her abdomen, but then last year the tube placed was too loose. I was told it was the Small but the thing was sticking way out from her abdomen. When she would go to defecate, it would come out to the first coil. I would say "Ellie fix your tube!" and she'd push it back in. It wasn't a horribly huge deal because she wears an abdominal binder (see this post) so it was keeping it in place. Nonetheless, it was a defective tube because it was labeled as a Small in the sterile package but it wasn't actually a small. With a tube that is too loose, there was stool leakage around the site which lead to skin breakdown. She has alway had leaking but this was a bit excessive. Think about a baby in diapers, they are at risk for skin breakdown and yeast infections. Preventatively, I would use Critic-Aid-AF around the site and keep covered with 4x4 gauze folded into quarters.
This was Ellie's tube from last year - notice how far it sticks out.
Even with all the preventative care, such a moist environment would lead to skin breakdown, like what you would see with a diaper rash and eventually infection. Typically, I would slap on some diaper cream. Well maybe not slap, but very carefully and gentle apply. I prefer Boudreaux butt paste, but really any diaper cream with zinc works. If that didn't resolve it, then adding some Lotrimin cream - yes the athlete's foot medicine- twice a day for 2 weeks would also help. Unfortunately, my skin sensitive little Bearity-Bear would still occasionally need us to whip out the big guns in the form of an oral antibiotic such as Keflex and once she needed oral Diflucan because it was yeast and bacterial. (Note: Ellie is notorious for getting infections in general, not just at her cecostomy site)
Left: Just after Ellie had her ostomy made, she had a bad reaction to the dressing adhesive
Right: excessive drainage saturated the gauze dressing resulting in skin irritation.
This is a combination of bacterial and yeast infection. She required both an oral antibiotic (Keflex) and an antifungal (Diflucan) to clear this up.
WHEN THE TUBE IS TOO SMALL
Guess what happens when you have a child going through a massive growth spurt? Any guesses? Just two months ago, Ellie had her annual tube replacement. She also packed on a bit of weight since then and all the sudden she developed this soft tissue swelling adjacent to the tube seemingly overnight. I panicked and was worried about a parastomal hernia (a hernia near an ostomy), which is actually not an uncommon thing. After a quick trip to the Bowel Clinic where she got to visit with her beloved Dr. R, the hernia was thankfully ruled out. Yes, the little Turkey still loves her doctors. Ellie's tube is officially too small/short. It is creating an indentation into her abdomen and causing soft tissue swelling and irritation. She is starting to have the beginnings of a pressure ulcer where the tube is digging into that swelling. I am now applying Meriplex, a silicone foam bandage under her tube to protect the skin until Interventional Radiology can fit her in for a new, larger tube. I am so frustrated because she *just* got this current Chait Trapdoor and now we need to sedate her again! Of course, my medical frequent flyer kiddo just takes all of this in stride. As long as she still can get her salad with broccoli (she's an odd duck) once she is home, she is a happy camper.
Soft tissue swelling due to the tube being too small. You can see how the tube is pushing into her abdomen. She has a Stage 1 pressure ulcer forming right where the tube is rubbing against the swelling.
As usual, it's fun times over in our household! Fingers crossed that I hear from IR soon. Our children's health system in Austin has only ONE interventional radiologist now and so the wait may be a while.
More on Cecostomies:
While this is a Down syndrome related blog, many of the health issues and psychiatric illnesses discussed here are unique to Ellie and not necessarily related to her having Ds.* Please see more information under the Disclaimers tab.