As someone with a diagnosed anxiety disorder, it wasn't very difficult for the usual worrying and feelings of anxiousness to transcend into full blown panic mode complete with heart palpitations, nausea, sweating, and feeling of impending doom. Then how the irrational suddenly becomes the rational.
*I apologize in advance for some missing photos - I used Photobucket for free as a means to store my photos and they are now holding a few hundred pics of mine for hostage unless I pay for an expensive plan and I also managed to lose half my photos from my computer*
 |
Then even more worrisome for me because it involve my baby, Ellie's surgery - the lingual tonsillectomy and glossectomy- which was going to commence exactly one week after my injection. By the Friday before Monday's procedure, I had talked myself into believing that because I worried, fretted, and had horrid dreams about all the "what ifs"related to all that could go wrong with Bear's surgery and recovery, that I worried all possible complications away. Of course, then I had myself thinking "well now I just jinxed it and something is going to go horribly wrong!"
As with most things, I worried for nothing. My shot was awesome with a minimal flare up followed by 50% pain relief and 75% decreased numbness/tingling. Ellie's procedure went well and she had a relatively smooth recovery.
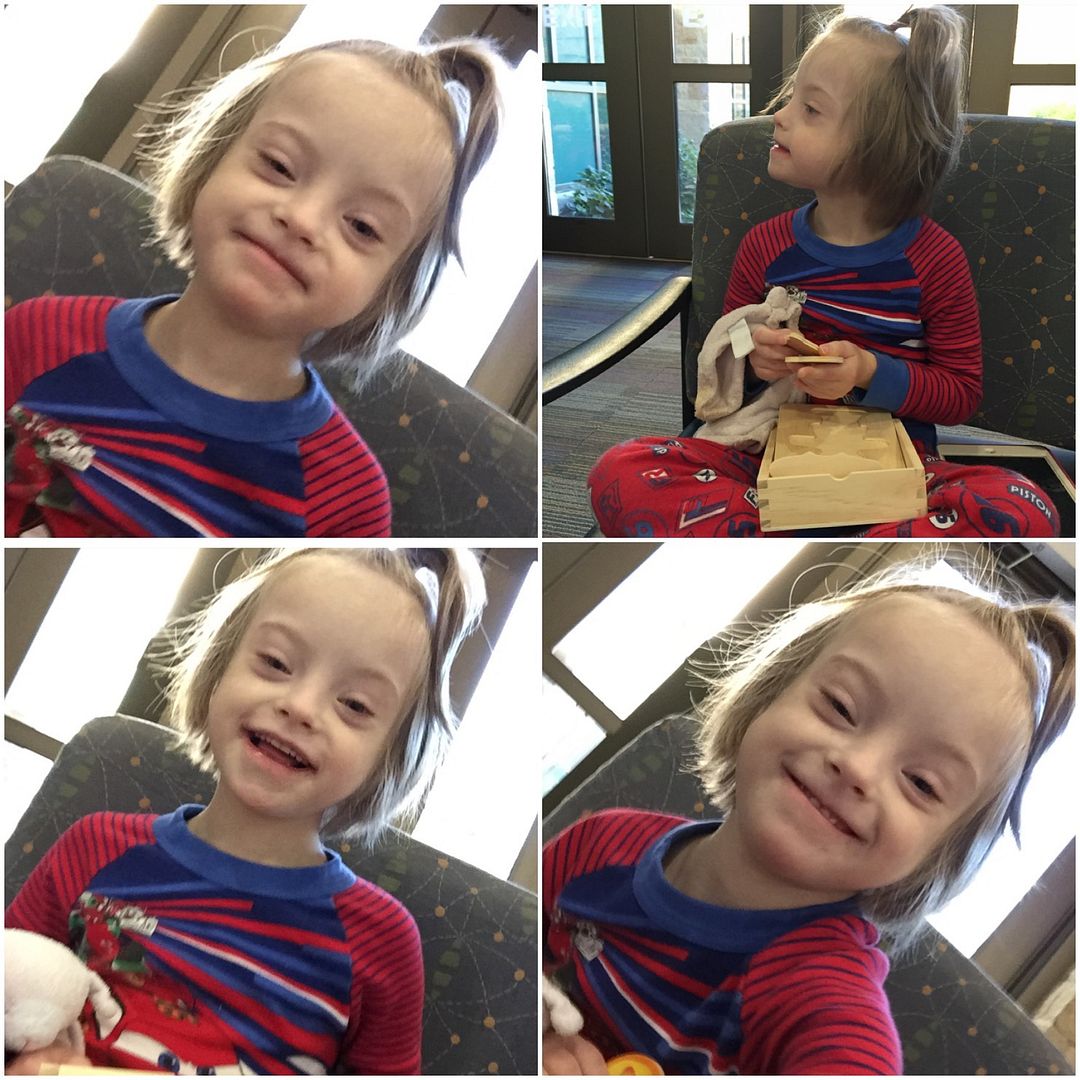 |
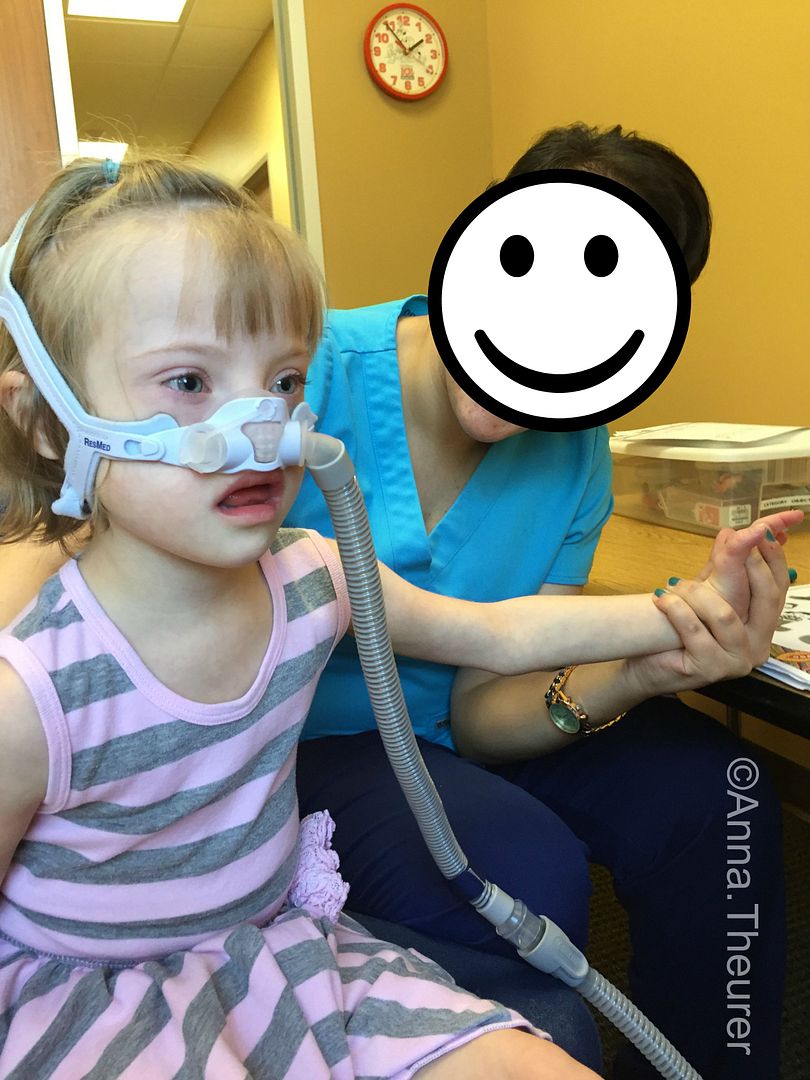
| Pre-operative waiting room Selfies |
Ellie's surgery lasted approximately 1.5 hours and she was a little stinker pants coming out of anesthesia. Then for the next two hours she was agitated and screaming bloody murder. Kicking, hitting and using her teeth to pull off the sock that was taped around her ankle. The sock that was covering her pulse oximetry monitor around her toe - the little thing that measures the oxygen saturations in the blood (normal is 98-100%). Given the thrashing that was already making it difficult of the pulse ox monitor to function proper, I respectfully asked if we could do spot checks every x number of hours rather than continuous monitoring and the doc looked weary. I totally understand seeing as the child just had her upper airway carved on! Yet, after spending just 5 minutes in the room with the Tasmanian Devil, the doc said "take it off and check her every 4 hours".
 |
| Busting out! Poor thing was feeling pretty cruddy, but she was happy to be headed home after a night in the hospital. |
I was extremely concerned about how things were going to go overnight- would she require oxygen since she is so swollen? Would she be in a lot of pain? Would she sleep at all? Again, it was needless worry for our Bearity Bear had oxygen saturations from 91-94% for the entire night!!! To me, that is proof that her surgery was a success because pre-surgery, she would sit at 81% for most of the night.
 |
| Play-doh pajama time with Daddy! Her cheeks were pretty swollen. |
A traditional tonsil and adenoidectomy recovery usually takes 7-10 days with an increase of pain around day 5-10 depending on when the scabs slough off (it was day 6 for Ellie a few years ago). With the lingual tonsils, there is less raw space and as such, less pain. The surgeon stated that normal recover for a lingual tonsillectomy is 5-7 days. Ellie's recovery took about 6 days with her returning to school the following Monday. I would say that post-op day 3 (Thanksgiving day, of course) was by far the worst where we had a hard time controlling her pain and that left her miserable, crying and rather agitated. As for the glossectomy, the tongue heals quickly - in a manner of 4-5 days. It did give her some seriously rank breath that lasted nearly 2 weeks - as in enough to pass out from if she were to breath on you! She is still snoring a bit, but I believe that is because she has some drainage and congestion due to her throat and tongue healing. We will have a follow-up sleep study in about 3 months to re-evaluate her sleep apnea.
So that was our November and now I can hardly believe that December is already here and soon 2016!
Follow us on Facebook! https://www.facebook.com/pages/The-Chronicles-of-Ellie-Bellie-Bear/216738345037166