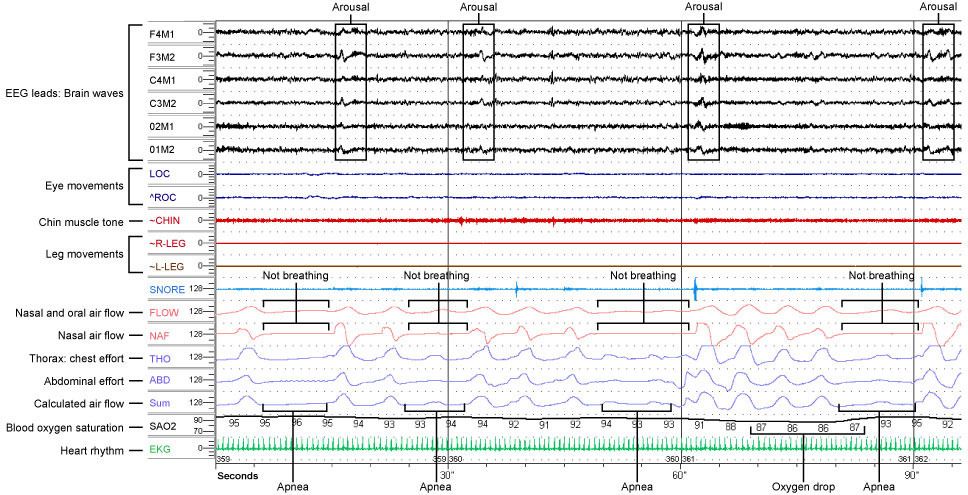
This is a follow up to Part 1: Polysomnography, Ellie's sleep study results, and OSA
The sleep study results landed Ellie with the official diagnosis of Obstructive Sleep Apnea with hypoventilation and oxygenation instability. Isn't that a mouthful?
Obstructive sleep apnea [OSA] and sleep disordered breathing [SDB] can have a huge impact on health. Actually, it can be very detrimental to one’s well-being. I still shutter when I think about what Ellie is at risk for if we do not treat her OSA.
The symptoms above are what we in the health care field refer to as "red flags". Some of the symptoms may mean nothing at all or may signal a sleep disorder. Yes, snoring is a sign of OSA, but not everyone who snores has OSA and not everyone who has OSA snores. That being said, chocking and gasping while sleeping is a neon sign indicative of OSA.
In addition to the signs listed above, kids can present with a few other symptoms (Ellie's are in purple):
- anger control issues
- difficulty swallowing
- irritability
- daytime sleepiness
- frequent runny nose
- mental brain fog
- hyperactivity
- impulsivity
- inattentiveness
- poor school performance
- memory loss
- headaches
- learning difficulties
 |
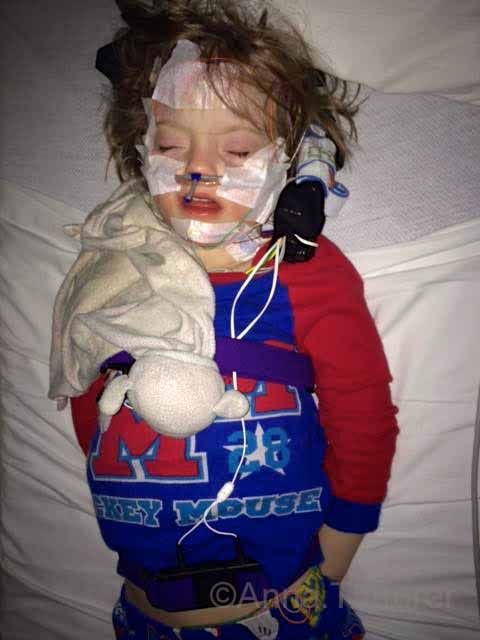
| This pic is from 2 years ago before her T & A. Notice that she is propping herself up or sitting up to sleep? These are also signs of sleep apnea in children. |
If you have been following this blog for any amount of time, you know that my daughter has severe ADHD and had shown signs prior to turning 3 years-old. You also know that when she has poor sleep, it is like ADHD on steroids—as in it is like she never took her Adderall. Her ability to function at school is pretty much nonexistent. She has trouble participating in class. Trouble sitting in circle time, lunch, art, music, therapy. Trouble concentrating and following directions. Impaired social interaction as she is “grabby, impulsive, irritable”.
In fact, studies (several posted in the medical journal Pediatrics between 2009-2013) suggest that there is a blurring of lines between ADHD and OSA. According to the American Sleep Apnea Association, at least 25% of children misdiagnosed with ADHD actually have a sleep disorder, specifically obstructive sleep apnea. This may be because poor sleep may damage neurons within the prefrontal cortex of the brain. I have no doubt that Ellie’s sleep apnea and early wakings manifest as ADHD behaviors. All of that being said, I do believe that she has underlying ADHD just because of our family history. It makes me wonder though, if we treat her OSA and we treat her ADHD, how well will she do in school? How will her friendships evolve? How will our home life change and be improved?
 |
| Photo: ADHD Caregiver Day |
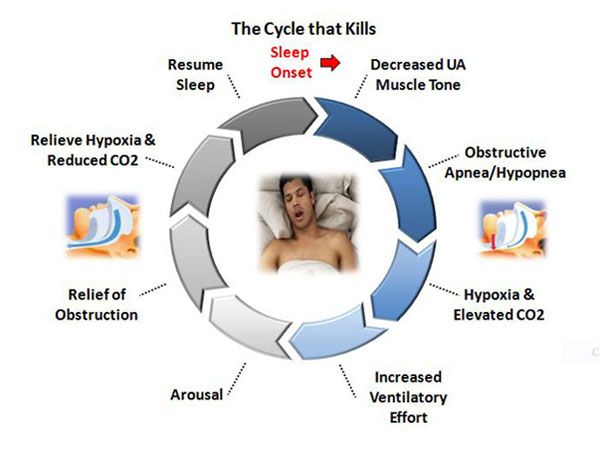
This goes beyond behavior though. Obstructive Sleep Apnea MUST be treated. It CANNOT be ignored.
Untreated OSA and the resulting high levels of inhaled CO2 and poor oxygenation can lead to:
- Increased heart rate and blood pressure
- Cardiovascular disease
- Increased risk for stroke
- Increased blood pressure
- Unstable blood glucose and insulin levels, leading to diabetes
- Memory loss
- Kidney problems
- Hormonal imbalance, especially with testosterone
In children, the usual culprits are enlarged tonsils and adenoid obstructing the upper airway. Nearly 2 years ago, this April, Ellie had a tonsillectomy and adenoidectomy [T&A]. She had a never ending sinus infection that was resistant to antibiotics and nasal sprays and it lasted months. She also had frequent ear infections that have required a set of ear tubes every 6-9 months. In those last 2 months leading up to her surgery, she was propping herself up to sleep. The T and A essentially cured her. After surgery, she didn’t have a sinus infection for 11 months. ELEVEN months! Ellie’s last set of ear tubes was in April 2013.
Sadly, all of that has changed. This past August is when she started up again with the recurrent, frequent sinus infections. August is also when her sleep issues started. She had fluid in her ears this past fall and an ear infection around Christmas. In December, I asked her ENT doc if her adenoid might have grown back. . . I was told it is rare and too soon. We were advised to wait until the summer and if she was still having sinus issues, we would reassess.
Oh yes, I did say it. THE ADENOID CAN GROW BACK! Yes, it isn’t common, but I laugh in the face of low percentages and low risk. After all, my odds ratio of having a child with Down syndrome was 1/1300. A 2011 study in Laryngoscope, show the rate of adenoid regrowth requiring a secondary adenoidectomy to be 1.3%. Another study in the International Journal of Otolaryngology revealed that those with adenoid regrowth tended to be younger at the age of their initial adenoidectomy as well as had a much larger adenoid than the general population. Ellie was 3.5 years-old at the time of her T&A and I was informed that her adenoid was “very massive with extreme crusting” aka large and nasty.
Ellie’s Treatment Plan :
- Follow up with ENT to rule out adenoid regrowth and palate abnormalities.
- If there is no adenoid regrowth, begin desensitization for CPAP (more on that later.)
- If CPAP is not tolerated, discuss further surgical options dependent upon cause of obstruction a. Palate Surgery for long palate obstruction or b. Genioglossus advancement aka base of tongue advancement surgery. Again, more on this later
Ellie’s Sleep Doc wanted her seen by ENT the week we got her results (2/9) or last week. Unfortunately, her ENT is out of town for the rest of this month. Thankfully, ENT and sleep doc coordinated and made sure the Ellie is seen the first day Dr. Z is back in office. So on March 3rd, Ellie will have her ENT visit. Meanwhile, we have that many more days until we get answers and even longer before we can treat her OSA.
Bring on the coffee!
Part 1: Polysomnography, sleep study results, and obstructive sleep apnea
Tonsil and Adenoid Removal (T&A) Recovery Tips
 |
| From a few years ago--I want to go back to sleeping! |
Follow us on Facebook!
http://www.facebook.com/annatheurerfitness
https://www.facebook.com/pages/The-Chronicles-of-Ellie-Bellie-Bear/216738345037166